Significance
The hierarchical organization of cortical systems is a fundamental concept in the field of neuroscience. It’s the idea that our brain’s functioning is structured along a hierarchical axis, with unimodal sensorimotor areas at one end and transmodal association areas at the other. This hierarchical organization is believed to enable the integration of sensory signals with a broad range of interoceptive and exteroceptive information, which is crucial for complex cognitive processes. Disturbances in this hierarchical system have been linked to adverse cognitive and clinical outcomes. Psychosis, a condition characterized by a detachment from reality, hallucinations, and delusions, is thought to be a result of impaired brain connectivity and the disruption of higher-order cognitive processes. Patients with psychosis often exhibit sensory deficits and difficulties in executive control and attention, which imply disruptions in the hierarchical signaling between cortical systems.
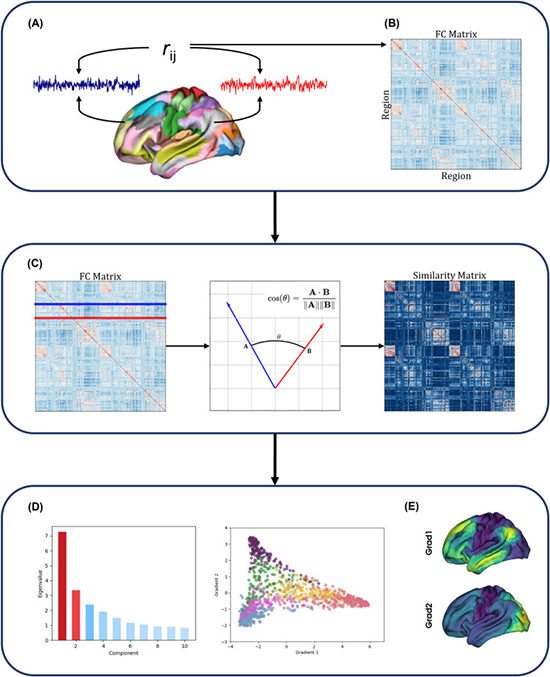
In a new study recently published in the peer-reviewed Journal Biological Psychiatry: Cognitive Neuroscience and Neuroimaging, led by a team of researchers including Alexander Holmes, Priscila Levi, Yu-Chi Chen, Sidhant Chopra, Kevin M Aquino, James Pang, and Professor Alex Fornito from Monash University in Australia, discussed the role of cortical organization in the development of psychiatric disorders, particularly schizophrenia. To investigate the hierarchical organization of cortical function, the researchers employed advanced dimensionality reduction techniques and resting-state functional magnetic resonance imaging (fMRI). This technique allowed them to decompose the inter-regional functional coupling into orthogonal axes of variation, providing insights into the hierarchy of cortical functions. The primary gradient was found to span from visual and sensorimotor areas to the default mode network (DMN) and other transmodal regions, consistent with classical descriptions of sensory-fugal cortical organization. The secondary gradient, on the other hand, differentiates sensorimotor areas from visual areas.
The study focused on two independent cohorts: one comprising early-stage psychosis patients and another with individuals diagnosed with established schizophrenia. The researchers aimed to determine whether disruptions in hierarchical cortical organization are present from the earliest stages of psychosis or if they emerge only with prolonged illness. The hypothesis was that both early psychosis and schizophrenia patients would display disrupted organization of the primary sensory-fugal gradient, characterized by a reduced functional differentiation between sensorimotor and transmodal association areas.
In the early psychosis cohort, the researchers observed that both healthy controls and early psychosis patients exhibited primary and secondary gradients. Importantly, there were no significant differences in the variance in functional coupling explained by these gradients between the two groups. This indicates that the primary sensory-fugal gradient is largely unaffected in early psychosis. This finding challenges the notion that disruptions in cortical organization are present from the very outset of psychosis.
In contrast, the cohort with established schizophrenia displayed a notable disruption. While the variance in functional coupling explained by the gradients did not significantly differ between healthy controls and schizophrenia patients, the latter group showed significantly lower scores in the visual network along the secondary gradient. This means that individuals with schizophrenia exhibit reduced differentiation between visual regions and opposing sensorimotor areas. This disrupted differentiation may be linked to perceptual disturbances and hallucinations.
The authors’ results also revealed that the disrupted gradient architecture in schizophrenia had a significant impact on the macroscale network organization. There was reduced between-network dispersion, particularly between the Visual network and other networks. Furthermore, there was a reduced within-network dispersion in several networks, including the Visual, Dorsal Attention, Limbic, and Frontoparietal networks. These findings suggest that the boundary between different sensory modalities is blurred in schizophrenia, impacting the organization of the cortex.
The research team investigated even further, exploring the clinical correlates of disrupted cortical organization in schizophrenia. It found strong associations between changes in between-network gradient dispersion and clinical outcomes. Increased between-network dispersion was associated with elevated scores on clinical measures related to negative symptoms and flattened affect, while decreased between-network dispersion was associated with elevated scores on clinical measures related to positive and general symptoms, including delusions and thought disorder.
In conclusion, the authors challenged previous assumptions about the nature of cortical organization disruptions in psychosis, particularly schizophrenia. Contrary to expectations, early psychosis patients did not exhibit significant disruptions in the primary sensory-fugal gradient. Instead, the disruption was primarily observed in established schizophrenia patients, affecting the secondary visual-to-sensorimotor gradient. The findings have significant implications for our understanding of how the brain’s hierarchical organization is affected in schizophrenia. It appears that disruptions are subtle and emerge as the illness progresses. The clinical correlates of these disruptions further underscore the importance of understanding cortical organization in the context of psychiatric disorders. This research opens up new avenues for exploring the relationships between cortical organization and the symptoms of schizophrenia, which may ultimately lead to more targeted and effective treatments for this challenging condition.
Reference
Alexander Holmes, Priscila T. Levi, Yu-Chi Chen, Sidhant Chopra, Kevin M. Aquino, James C. Pang, Alex Fornito, Disruptions of Hierarchical Cortical Organization in Early Psychosis and Schizophrenia, Biological Psychiatry: Cognitive Neuroscience and Neuroimaging, 2023,
Go To Biological Psychiatry: Cognitive Neuroscience and Neuroimaging
 Medicine Innovates Medicine Innovates: Delivering innovations in medicine to the world for better health and prosperity
Medicine Innovates Medicine Innovates: Delivering innovations in medicine to the world for better health and prosperity

